CMS Expands RPM Coverage: New Reimbursement Codes 2026

In a landmark announcement poised to reshape the landscape of chronic disease management and remote healthcare delivery, the Centers for Medicare & Medicaid Services (CMS) has unveiled a series of new reimbursement codes for Remote Patient Monitoring (RPM). These pivotal changes, set to take effect on January 1, 2026, promise to significantly expand coverage for a wide array of chronic conditions, opening new avenues for patient care and provider engagement. This comprehensive guide delves into the specifics of these new CMS RPM Reimbursement Codes, exploring their implications for healthcare providers, patients, and the broader healthcare ecosystem.
The advent of these updated codes underscores CMS’s enduring commitment to integrating innovative technologies into mainstream healthcare. Remote Patient Monitoring has long been recognized for its potential to enhance patient outcomes, reduce hospital readmissions, and empower individuals to take a more active role in managing their health from the comfort of their homes. With the 2026 expansion, CMS is not merely tweaking existing policies; it is fundamentally broadening the scope and applicability of RPM, making it an accessible and viable option for millions more Americans living with chronic illnesses.
Understanding these new CMS RPM Reimbursement Codes is paramount for any healthcare organization looking to leverage the full potential of remote care. From primary care practices to specialized clinics, the ability to accurately bill for RPM services will be crucial for sustainability and growth. This article will break down the new codes, clarify the eligibility criteria, discuss the types of services covered, and provide strategic insights for successful implementation.
The Evolution of Remote Patient Monitoring and CMS’s Role
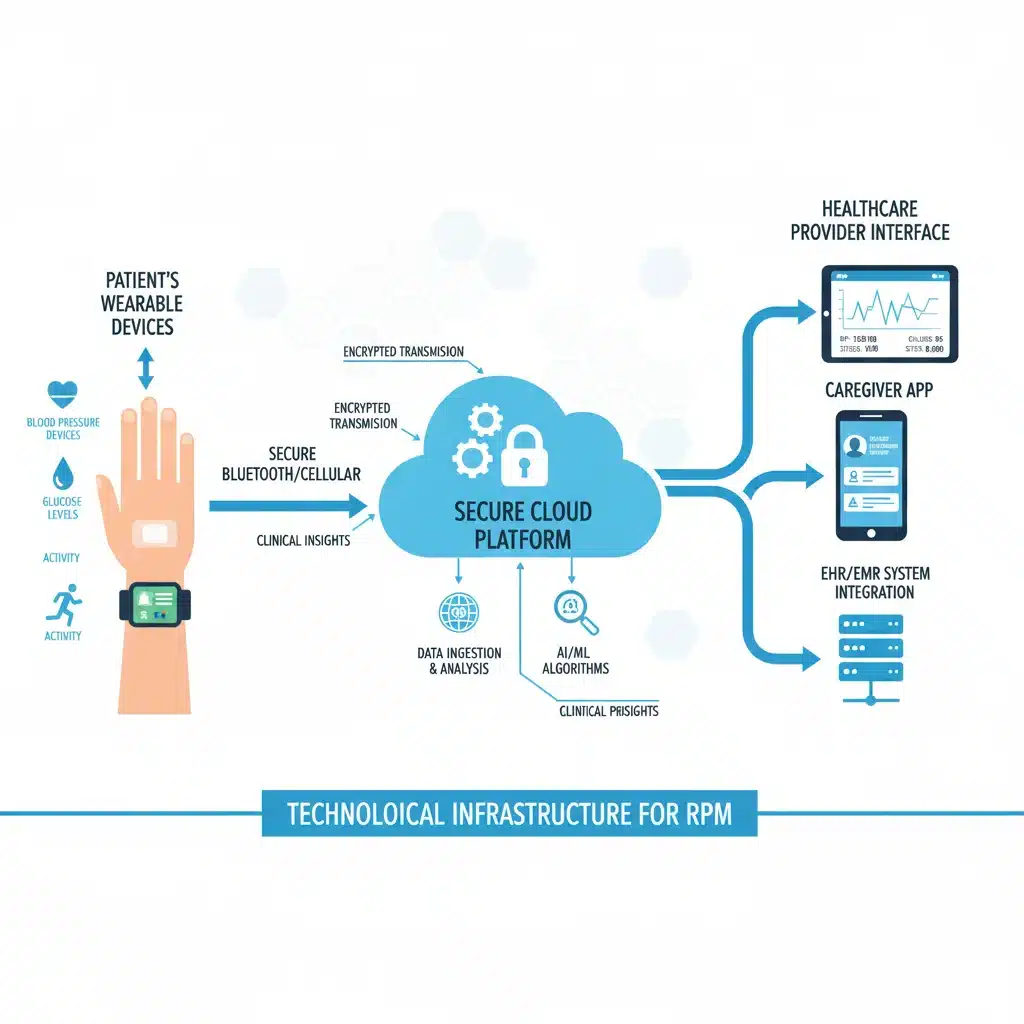
Remote Patient Monitoring, often referred to as RPM, involves the use of digital technologies to collect health data from individuals in one location and electronically transmit that information securely to healthcare providers in a different location for assessment and recommendations. This technology has proven invaluable for managing chronic conditions such as hypertension, diabetes, heart failure, and chronic obstructive pulmonary disease (COPD).
CMS has been instrumental in the gradual integration of RPM into the healthcare system. Initially, reimbursement for RPM services was somewhat limited, often tied to specific scenarios or bundled with other services. However, the COVID-19 pandemic accelerated the adoption of telehealth and RPM, highlighting their critical role in maintaining continuity of care when in-person visits were challenging. This period served as a powerful testament to RPM’s efficacy and convenience, prompting CMS to re-evaluate and expand its reimbursement policies.
The forthcoming 2026 changes represent a significant leap forward. They reflect CMS’s recognition of RPM not just as a temporary solution but as an integral, long-term component of modern healthcare delivery. By expanding the CMS RPM Reimbursement Codes, the agency aims to remove financial barriers that have previously hindered widespread adoption, encouraging more providers to offer these services and more patients to benefit from them.
Key Drivers Behind the Expanded Coverage
Several factors have influenced CMS’s decision to expand RPM coverage:
- Aging Population and Chronic Disease Burden: As the U.S. population ages, the prevalence of chronic diseases continues to rise. RPM offers an efficient way to manage these conditions, preventing exacerbations and improving quality of life.
- Technological Advancements: The rapid evolution of wearable devices, smart sensors, and secure data platforms has made RPM more accurate, user-friendly, and cost-effective than ever before.
- Cost-Effectiveness: By enabling proactive management and early intervention, RPM can significantly reduce the need for expensive emergency room visits and hospitalizations, leading to overall healthcare cost savings.
- Patient Preference: Many patients prefer the convenience and comfort of managing their health from home, especially those with mobility issues or living in rural areas with limited access to specialists.
- Lessons from the Pandemic: The unprecedented circumstances of the COVID-19 pandemic solidified RPM’s role as a resilient and essential component of healthcare infrastructure.
Understanding the New CMS RPM Reimbursement Codes for 2026
While the precise details of every new code and its specific descriptors are still being finalized and will be released in official CMS documentation, the overarching theme is a broader definition of what constitutes reimbursable RPM services and an expansion of eligible chronic conditions. Here’s a general overview of what providers can anticipate:
Expanded Eligibility Criteria for Patients
Previously, RPM eligibility was often narrowly defined. The 2026 updates are expected to:
- Broaden Chronic Condition Scope: Expect a wider range of chronic conditions to be explicitly covered, moving beyond the most common ones to include a more comprehensive list of long-term health issues that benefit from continuous monitoring.
- Reduced Barrier to Entry: CMS may relax certain ‘face-to-face’ requirements or initial encounter stipulations, making it easier for providers to initiate RPM services for eligible patients.
- Focus on Medical Necessity: The emphasis will remain on medical necessity, ensuring that RPM services are clinically appropriate and contribute meaningfully to patient care plans.
New and Revised Service Codes
The core of the CMS RPM Reimbursement Codes expansion lies in the introduction of new codes and revisions to existing ones. These are likely to address:
- Device Provision and Setup: New codes might specifically delineate reimbursement for the provision of RPM devices to patients and the initial setup and patient education required for their use.
- Data Transmission and Monitoring: Expect refined codes for the collection, transmission, and initial review of RPM data over specified periods (e.g., daily, weekly, monthly).
- Interactive Communication and Management: This is a critical area. New codes are anticipated to better compensate for the clinical staff time spent on interactive communication with patients and caregivers, interpretation of data, and subsequent management decisions based on RPM insights. This includes time spent on patient coaching, medication adjustments, and care plan modifications.
- Complex RPM Services: There might be new codes or modifiers for more complex RPM scenarios, such as those involving multiple chronic conditions, advanced analytical interpretation, or integration with other telehealth services.
- Specific Disease Management Modules: Potentially, CMS could introduce codes tailored to specific disease management protocols facilitated by RPM, offering more granular billing options.
Providers will need to meticulously review the final rule when it is published to understand the exact definitions, time requirements, and documentation standards associated with each new or revised code.

Implications for Healthcare Providers
The expanded CMS RPM Reimbursement Codes carry profound implications for healthcare providers across the spectrum. Preparing for these changes now will be critical for seamless integration and maximizing benefits.
Increased Revenue Opportunities
For many practices, the primary draw of expanded RPM coverage will be the potential for increased revenue. By offering reimbursable RPM services, providers can create new revenue streams, improve their financial health, and invest further in technology and staff. This is particularly beneficial for practices serving a high volume of patients with chronic conditions.
Enhanced Patient Engagement and Outcomes
Beyond financial incentives, RPM significantly enhances patient care. Continuous monitoring allows for:
- Early Detection of Issues: Providers can identify concerning trends or acute changes in a patient’s health status much faster than with periodic office visits, enabling timely interventions.
- Personalized Care Plans: Real-time data provides a clearer picture of a patient’s health in their daily life, allowing for more precise and personalized care plan adjustments.
- Improved Medication Adherence: RPM can help track the impact of medications and identify issues with adherence, leading to better therapeutic outcomes.
- Greater Patient Empowerment: Patients often feel more engaged and in control of their health when they are actively monitoring their vital signs and communicating with their care team.
Operational and Workflow Adjustments
Implementing or expanding RPM services will require operational adjustments:
- Staff Training: Clinical and administrative staff will need training on new RPM technologies, data interpretation, patient communication protocols, and, crucially, accurate billing procedures for the new CMS RPM Reimbursement Codes.
- Technology Integration: Practices will need robust RPM platforms that can integrate with their Electronic Health Records (EHR) systems, ensuring seamless data flow and efficient documentation.
- Workflow Optimization: Developing clear workflows for patient onboarding, device distribution, daily monitoring, alert management, and follow-up communication will be essential.
- Compliance and Documentation: Adhering to CMS guidelines for documentation will be vital to avoid claim denials. This includes detailed records of patient consent, device usage, data reviews, and clinical interventions.
Addressing Health Equity
The expansion of RPM coverage also has the potential to address health equity concerns. By making remote care more accessible and affordable, CMS can help bridge gaps in care for patients in rural areas, those with limited transportation, or individuals who struggle to take time off work for appointments.
Strategic Planning for the 2026 CMS RPM Reimbursement Codes
Given the significant lead time, healthcare organizations have a unique opportunity to strategically plan for the 2026 changes. Proactive measures can ensure a smooth transition and maximize the benefits of the expanded CMS RPM Reimbursement Codes.
1. Stay Informed and Monitor CMS Updates
The first step is continuous monitoring of official CMS announcements. Subscribe to CMS newsletters, regularly check their website for proposed and final rules, and engage with industry associations that provide updates and interpretations of new policies. The devil will be in the details of the final rule.
2. Assess Current RPM Capabilities
Conduct an internal audit of your current RPM infrastructure, if any. Evaluate:
- Technology: Is your current RPM platform scalable? Does it offer the necessary features for expanded services? How well does it integrate with your EHR?
- Staffing: Do you have sufficient clinical staff (nurses, medical assistants) to manage an increased volume of RPM patients? What training gaps need to be addressed?
- Workflows: Are your existing workflows efficient? Can they accommodate new patient cohorts and expanded service offerings?
- Billing Expertise: Is your billing department prepared to handle the new CMS RPM Reimbursement Codes and their specific requirements?
3. Invest in Robust RPM Technology
Choosing the right RPM platform is crucial. Look for solutions that offer:
- Device Agnosticism: Compatibility with a wide range of FDA-approved devices.
- User-Friendliness: Easy for both patients and clinical staff to use.
- Interoperability: Seamless integration with your EHR and other health IT systems.
- Data Analytics: Tools for interpreting data, identifying trends, and generating actionable insights.
- Security and Compliance: Adherence to HIPAA and other relevant data privacy regulations.
- Scalability: Ability to grow with your practice’s RPM program.
4. Develop Comprehensive Training Programs
Invest in thorough training for all staff involved in RPM. This should cover:
- Clinical Protocols: How to onboard patients, educate them on device use, interpret data, and respond to alerts.
- Communication Skills: Best practices for remote patient communication and engagement.
- Documentation Standards: Ensuring all required information is accurately recorded to support billing.
- Billing and Coding: In-depth training on the new CMS RPM Reimbursement Codes, modifiers, and common billing scenarios.
5. Refine Documentation and Billing Processes
Accurate documentation is the bedrock of successful reimbursement. Establish clear guidelines for:
- Patient Consent: Obtaining and documenting informed consent for RPM services.
- Device Distribution Records: Tracking which devices are provided to which patients.
- Monitoring Logs: Detailed records of data collection periods and clinical staff time spent on monitoring and management.
- Clinical Notes: Comprehensive notes on patient interactions, data interpretations, and care plan adjustments.
Work closely with your billing team or a third-party medical billing service to ensure they are fully conversant with the new CMS RPM Reimbursement Codes and can submit claims efficiently and accurately.
6. Patient Education and Outreach
Successful RPM programs rely on active patient participation. Develop strategies for:
- Educating Patients: Informing eligible patients about the benefits of RPM and how it works.
- Addressing Concerns: Proactively addressing patient questions about technology use, data privacy, and their role in the program.
- Ongoing Support: Providing accessible support channels for patients encountering technical issues or needing assistance with their devices.
The Future of Remote Patient Monitoring Under Expanded CMS Coverage
The expansion of CMS RPM Reimbursement Codes effective January 1, 2026, marks a pivotal moment for healthcare. It signifies a robust endorsement from the nation’s largest payer for the value and efficacy of remote care technologies, especially in the context of chronic disease management.
This move is expected to catalyze further innovation in the RPM space. Device manufacturers will likely accelerate the development of more sophisticated, user-friendly, and integrated solutions. Software developers will continue to enhance platforms with advanced analytics, AI-driven insights, and improved interoperability. Moreover, the broader acceptance and financial viability of RPM will likely encourage more research into its long-term impact on various chronic conditions and patient populations.
For healthcare providers, the expanded coverage offers an unprecedented opportunity to modernize their practices, improve patient outcomes, and contribute to a more efficient and patient-centered healthcare system. It’s a call to action to embrace digital health solutions and integrate them strategically into existing care models.
Patients, particularly those grappling with the complexities of chronic conditions, stand to gain immensely. The ability to receive continuous, proactive care from the comfort of their homes can significantly enhance their quality of life, reduce the burden of frequent clinic visits, and empower them with greater control over their health journey. The new CMS RPM Reimbursement Codes will make this level of care accessible to a much broader segment of the population.
Conclusion
The announcement of new CMS RPM Reimbursement Codes effective January 1, 2026, is more than just a regulatory update; it’s a clear signal of the future direction of healthcare. Remote Patient Monitoring is no longer a niche service but a mainstream component of comprehensive chronic disease management. Healthcare providers who proactively prepare for these changes by investing in technology, training staff, and optimizing workflows will be best positioned to thrive in this evolving landscape.
By embracing these expanded opportunities, providers can not only enhance their financial stability but, more importantly, deliver superior, patient-centric care that leverages the power of technology to improve health outcomes for millions. The countdown to 2026 has begun, and the time to strategize and adapt for the new era of RPM is now. Stay tuned for the final detailed CMS guidelines to ensure full compliance and maximize the benefits of these transformative changes.





